1. Define vital capacity. What is its significance?
Solution:
Vital capacity can be defined as the maximum volume of air a person can breathe in post a forced expiration.
Significance of vital capacity:
(i) It depicts the maximum amount of air that can be converted or renewed in the respiratory system in a single respiration
(ii) The excess quantity of inhaled air represents the maximum amount of oxygen available for glucose-oxidation. This way more energy is available for the body.
2. State the volume of air remaining in the lungs after a normal breathing.
Solution:
It can be stated by the functional residual capacity (FRC). FRC is the volume of air that remains in the lungs after a normal expiration. The functional residual capacity is both the expiratory reserve volume (ERV) and residual volume (RV).
The expiratory reserve volume is the maximum volume of air which can be exhaled post a normal expiration which is approximately1000ml-1500ml. The residual volume is the volume of air that remains in the lungs after maximum expiration which is about 1100ml to 1500ml.
Hence,
FRC = ERV + RV
≅ 1500 + 1500 = 3000 ml
Thus, the functional residual capacity of the lungs in human beings is nearly 2500 ml to 3000 ml
3. Diffusion of gases occurs in the alveolar region only and not in the other parts of
respiratory system. Why?
Solution:
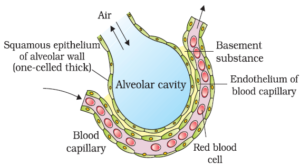
Alveoli are the small air sacs of the lungs that allow rapid gas exchange. These structures are specially built for the gas exchange process. The thickness of the alveolar membrane in total is lesser than a millimeter, while the outer surface of the alveolar membrane is in close proximity with the linkage of blood capillaries.
 `
`
The endothelial membrane of the blood capillaries and the alveolar membrane is distinguished by a fine basement substance. This fine barrier facilitates easy diffusion of the gases. The alveolar air that comes in close proximity with the blood capillaries has higer levels of pO2and lower levels of pCO2that promote the gas-diffusion. All these structural pluses that are found in alveoli is not present in any other structure of the respiratory system. Therefore, the gas diffusion phenomena occurs in the alveolar region only and not in any other part.
4.What are the major transport mechanisms for CO2? Explain.
Solution:
Carbon dioxide is liberated by a vigorously active tissue in the blood. On an average, every 100ml of blood accepts approximately 3.7ml of CO2from tissues.
In blood, carbon dioxide is carried in three forms:
1. Carbon dioxide as a simple solution
Nearly 5-10% of carbon dioxide of the total volume of blood is dissolved in plasma and is transported as a simple physical solution
2. Carbon dioxide as a bicarbonate ion
The partial pressure of carbon dioxide at the tissue site is high due to catabolism. Carbon dioxide diffuses in the blood and forms carbonic acid after reacting with water. This reaction occurs in the presence of the carbonic anhydrase enzyme. The reaction is as follows:
![]()
Carbonic acid dissociates into H+ions and bicarbonate. Some amount of bicarbonate ions is required to sustain the pH of blood. The hydrogen ions are used by the proteins, the remaining bicarbonate ions are picked up by the plasma.
3. Carbon dioxide as carbamino-haemoglobin
In tissues, when the partial pressure of oxygen is lower and the partial pressure of carbon dioxide is higher, the carbon dioxide loosely combines with the globin part of the reduced haemoglobin so as to form carbamino-haemoglobin. The reaction is as follows:
![]()
At the alveolar level, when pO2is higher and the pCO2is lower, the carbon dioxide dissociates from carbamino-haemoglobin. Therefore, carbon dioxide that is bound to haemoglobin is liberated in the alveoli.
5. What will be the pO2and pCO2in the atmospheric air compared to those in the alveolar air?
(i) pO2lesser, pCO2higher
(ii) pO2higher, pCO2lesser
(iii) pO2higher, pCO2higher
(iv) pO2lesser, pCO2lesser
Solution:
The pO2and pCO2in the atmospheric air compared to those in the alveolar air will be:
(ii) pO2higher, pCO2lesser
In a mixture of gases, each gas exerts a pressure known as partial pressure. These gases always diffuse across the pressure gradient. Oxygen permeates easily into the lungs when the level of pO2is higher in the atmosphere. Likewise, carbon dioxide can diffuse out of the body easily if the pCO2level is lower in the atmosphere.
6.Explain the process of inspiration under normal conditions.
Solution:
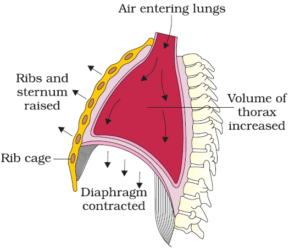
The process by which fresh air enters into the lungs is known as inspiration. When the intrapulmonary pressure (pressure in the lungs) is lesser than the atmospheric pressure, inspiration takes place. The muscles of the diaphragm, external intercostal muscles and abdominal muscles are referred to as the inspiratory muscles which bring about the process of inspiration.
The muscles of the diaphragm contract, pulling the diaphragm downwards to the abdominal cavity, causing it to become flat which results in an increase in the thoracic cavity in the anteroposterior direction. The contraction of the external intercostal muscles lifts up the ribs and the sternum resulting in the expansion of the thoracic chamber, in a dorso-ventral orientation.
This overall increase in the thoracic volume increases the pulmonary volume which in turn causes the decrease of pressure in the lungs. The atmospheric pressure expels air from outwards into the lungs. To compress the abdominal organs, the abdominal muscles relax that causes an escalation in the strength of the inspiration.
7.How is respiration regulated?
Solution:
The medulla region of the brain having the respiratory rhythm center, is chiefly responsible for the regulation process of respiration. The function performed by the respiratory rhythm center can be altered by the pneumotaxic center through signals to reduce the inspiration rate. The chemo sensitive area located near the respiratory centre is sensitive to hydrogen ions and carbon dioxide. This region then sends signals to alter the rate of expiration to eliminate compounds.
The levels of carbon dioxide and hydrogen ions in the blood is detected by the receptors located in the carotid artery and the aorta. As the carbon dioxide level increases, the respiratory centre sends nerve impulses for the required changes.
8.What is the effect of pCO2on oxygen transport?
Solution:
pCO2has a crucial role to play in the process of oxygen transport. As a result of low pCO2levels in the alveoli, oxygen tends to bind with the hemoglobin, to form Oxyhaemoglobin. Higher levels of pCO2and lower level of pO2in the tissues promotes the dissociation of oxygen from Oxyhaemoglobin. The level of pCO2is low at the surface of the lungs, here O2binds with the haemoglobin and dissociates at the tissue grade, where the level of pCO2is higher.
9.What happens to the respiratory process in a man going up a hill?
Solution:
As we go up higher, the altitude increases. At this altitude, the concentration of atmospheric oxygen is lesser, which means to say that the partial pressure of oxygen declines. This situation of inadequate oxygen-supply, demands more of oxygen. In order to increase the supply of oxygen to the blood, the man begins to breathe rapidly. Therefore, it causes an increase in the heart rate to be able to meet the demand of oxygen supply.
10.What is the site of gaseous exchange in an insect?
Solution:
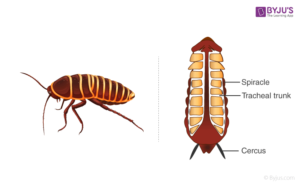
The respiratory organs of insects is trachea. Trachea has openings known as spiracles through which air enters. Spiracles are located on either side of the abdomen of the insect. A pair of spiracles are found on each segment of the abdomen. Furthermore, the trachea branches into smaller tubes until they reach the level of tissues. The oxygen that enters the trachea is exchanged by diffusion with the tissues. Simultaneously, carbon dioxide that reaches the trachea from the tissues is forced out of the body.
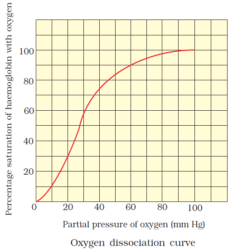
11.Define oxygen dissociation curve. Can you suggest any reason for its sigmoidal pattern?
Solution:
A graph attained when the percentage saturation of haemoglobin with oxygen is plotted against the partial pressure of oxygen.